A proactive safety culture contributes to patient safety. It is a culture in which everyone is alert to potential risks and in which action steps can be taken towards incident reporting without consequences, in an open atmosphere. A climate in which – by lowering the threshold – unsafe situations in care processes can be reported.
The safety culture ladder provides insight and demonstrable clarity into the degree to which an organization works in a safe manner. This blog describes how an organization can rank higher on the safety culture ladder, emphasizing the importance of open communication.
The safety culture ladder
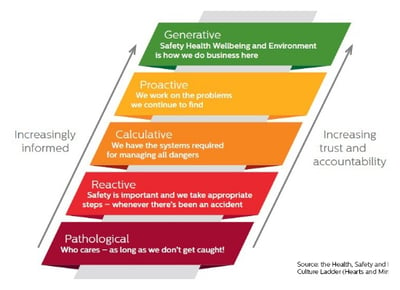 The safety culture ladder distinguishes five various types of safety culture (Generative, Pro-active, Calculative, Reactive and Pathological), see the visual.
The safety culture ladder distinguishes five various types of safety culture (Generative, Pro-active, Calculative, Reactive and Pathological), see the visual.
The higher the safety awareness is in an organization, the higher the score on the safety culture ladder. The ladder enables safety awareness in organizations to be continuously measured and improved.
A safety culture in denial can be found at the bottom of the safety ladder, under the term 'pathological'. Institutions with a safety culture in denial, truly live in denial – and do not want to waste time on safety, because they are convinced the healthcare they provide is safe...
Characteristics of a safety culture in denial
- The organization thinks it provides good healthcare.
- The environment to identify/report errors is unsafe.
- Professionals who report errors / unsafe incidents can count on repressive measures.
- Professionals who detect mistakes or have themselves made mistakes tend to hide these incidents from others including the Board and Inspectorate.
- Serious lack of confidence.
- Board has the erroneous impression that everything is proceeding smoothly.
- The question is not if a calamity will take place, but when.
Create a pro-active safety culture
In order to develop from a culture in denial into a reactive or even pro-active culture, more openness about and awareness of risk is a prerequisite. In a pro-active culture, care professionals can report incidents safely and without any fear of sanctions. Moreover, they can rely on the findings of analyses leading to focused enhancements that can be implemented throughout the institution. The role of management in this process determines its success. Management should demonstrate exemplary behavior in which commitment to and effort towards safety in healthcare is promoted. Open communication about improvements also plays an important role in this respect.
Management can make it clear in this way that the importance of learning from incidents and boosting healthcare safety takes center stage. But what if open communication is an issue itself?
Communication and leadership in healthcare
The tasks of management, departmental heads, team leaders and any other care professional who assumes a leadership role are complicated when stress, personality differences or other issues hinder communication. This does nothing to improve the cooperation needed to safeguard safety in healthcare. In order to improve safety culture, it is important that care professionals learn to communicate in an open fashion.
It should be possible that a nurse, a departmental medical student, or a fellow surgeon can express criticism. They must not assume that the doctor knows it all, but stand up and make themselves heard if they think that something is not right.
Research indicates that human error was the most significant cause of aircraft accidents in the Seventies and Eighties of the last century. Underlying causes are a lack of mutual communication, the influence of stress and fatigue on performance, too much hierarchy, a lack of assertiveness and overestimation of knowledge and skills. Based on these findings, the airline business started a Crew Resource Management (CRM) program to enhance the non-technical skills of cockpit and cabin staff.
Based on the well-known report called ‘To err is human’ by the Institute of Medicine (1999), this concept has been adopted by the healthcare sector. This concept is now referred to as Team Resource Management (TRM), because it is about collaboration within teams.
Team Resource Management in healthcare
In TRM training sessions, care professionals learn how to deal with certain procedures that enhance safety and efficiency in the healthcare sector. In these courses, attention is paid to team and cooperation skills as well as individual interpersonal communication skills such as giving feedback, engagement, assertiveness, etc. In a nutshell, it comes down to all the necessary tasks to enable teams to work together safely.
TRM skills can help operational teams to learn what is required to work together effectively and safely in the field of communication and leadership. In the TRM training sessions, teams learn how to communicate effectively by practicing how to cope in stressful situations in which communication can be key.
Teams should work on these skills regularly for the preservation of the fundamental instincts of healthcare safety and risk prevention by care professionals and teams.
Outcomes Team Resource Management
- Participants highly value TRM training sessions.
- The sessions have a positive impact on attitude and behaviour, primarily in those areas of giving and receiving feedback whereby more room is created for open communication.
- It improves the open ambiance and that has a positive impact on employee satisfaction.
Not much is known about the TRM outcomes, but various hospital examples indicate that both the number of serious complications and the mortality rates diminished, as well as a safer healthcare climate being recorded.
It’s all about open and structured conversation and cooperation. You make use of briefings and checklists and learn to give and take criticism.
How TPSC Cloud™ supports a safety culture
TPSC's online quality and risk management software platform (TPSC Cloud™) enables every supervisor and care professional to report incidents and bring them out into the open. Reports can be compiled simply and quickly at every desirable level, whereby incidents, risks and trends can be made visible real-time. These are used to discover points of improvement that are registered and monitored within the online improvement tracking system "Improve 2.0.". The software promotes learning and open communication about quality and safety.
Thereby, by applying online culture surveys you can measure the organizational culture and see which actions contribute to creating the desired safety culture.
Read the eBook about creating a healthcare safety culture
Like to know more about interventions that you can apply to create culture change? Download the e-book 'Safety is our joint effort!' about creating a healthcare safety culture:


%20(3)%20(1).jpg)


